“Just exercise” is common advice that’s helpful in theory, but it’s not always so simple if you live with rheumatoid arthritis. Stiff, swollen, and unpredictable joints can make working out a challenge. The difference-maker isn’t simply moving more. It’s moving in a way that respects inflammation, protects your joints, and helps you feel confident again.
That’s why aquatic therapy for rheumatoid arthritis is a game-changer. It is one of the best and safest ways to manage arthritis pain. A warm therapy pool provides support as you work to improve mobility, strength, balance, and walking. And when an Ivy Rehab physical therapist guides the plan, it’s not random laps or water aerobics. It’s goal-focused rehab built around your symptoms, your flare-up patterns, and what you want to get back to doing.

Why Aquatic Therapy Works for Rheumatoid Arthritis
Rheumatoid arthritis is an autoimmune inflammatory condition, which means joints can become painful, swollen, and stiff, sometimes with very little warning. Warm water creates a more forgiving environment for movement, making it feel more manageable during sensitive stretches. That’s one reason aquatic therapy for rheumatoid arthritis is often used as a low-impact option and a practical bridge back to the activity you remember. It can also help people with osteoarthritis, a condition that can wear down joints over time, making everyday movement feel achy and stiff.
Buoyancy Reduces Joint Pressure
Water supports part of your body weight. That can make it easier to practice walking, balance, and strengthening with less joint compression than you might feel on land.
For many people, buoyancy can help with:
- Moving more freely through painful joints.
- Taking pressure off the hips, knees, ankles, and the spine.
- Practicing better alignment without “guarding,” which is tensing up to avoid pain.
Your big win is not doing more for the sake of doing more. It’s building steadier movement that feels safer and more sustainable.
Warm Water Relieves Stiffness
Warm water can help muscles relax and support circulation, which can be especially comforting when stiffness is a regular part of your day. Many people notice their joints feel looser in the pool, so getting started doesn’t feel like such a negotiation.
Not a morning person? Pool sessions can be a gentler way to start your day. You still get the therapy your body needs. You just do it with less friction.
Water Resistance Builds Strength Gently
Water is supportive, but it’s not a free ride. It provides resistance in every direction, allowing you to improve flexibility and muscle strength without the need for heavy weights or high-impact loading.
That matters for rheumatoid arthritis because stronger muscles help support and stabilize joints. With your physical therapist’s guidance, you can build strength while minimizing common flare-up triggers, such as overexertion, moving too quickly, or using other muscles to compensate for weakness.
Safe Environment for Limited Mobility
If you deal with fatigue, balance concerns, instability, or fear of falling, the pool can feel like an ideal place to practice. Your Ivy Rehab physical therapist can adjust water depth, use support tools, and pace the session, so you stay challenged without feeling pushed past your limits.
Aquatic therapy leaves you feeling better equipped for life, not wiped out for the next two days.
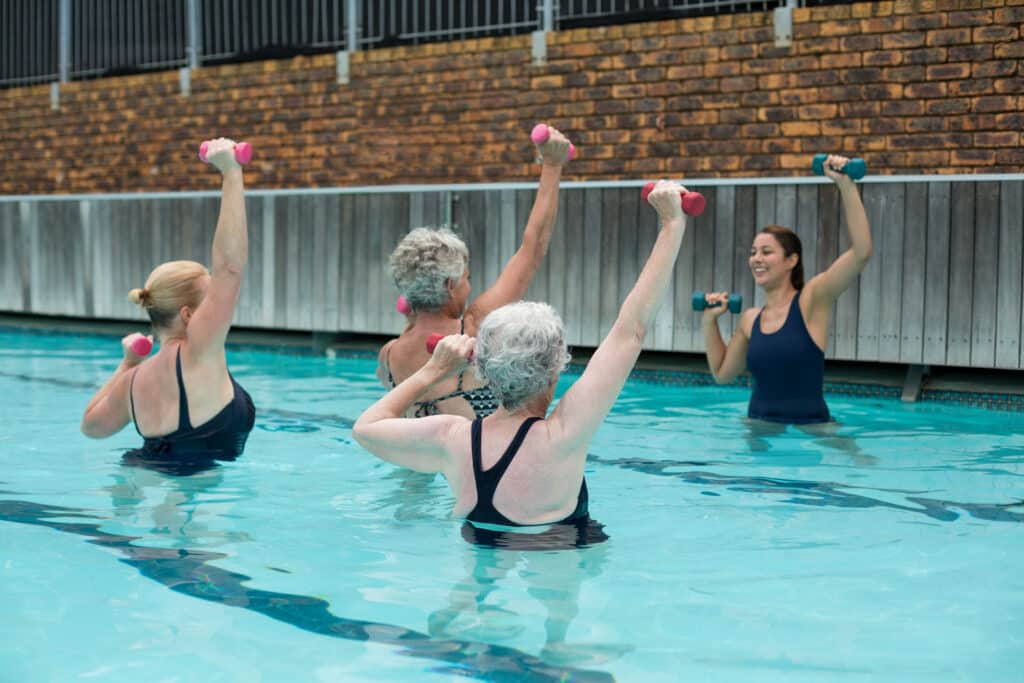
PT-Recommended Aquatic Exercises for Arthritis Relief
A helpful aquatic program isn’t about max effort. It’s about smart effort. The primary goal of aquatic therapy for rheumatoid arthritis is to focus on comfort-first motion, joint-friendly strength, and better function for everyday tasks.
Below are examples of movements commonly used in the pool and guided by a physical therapist. Your plan should be adjusted based on the joints involved, your balance and endurance, and whether you’re experiencing a flare-up.
Water Walking (Slow and Controlled)
Water walking is a simple starting point that can deliver meaningful benefits. Your physical therapist may adjust speed, posture, and water depth to support painful joints while helping you practice proper movement techniques.
This can help:
- Improve gait mechanics and confidence with walking.
- Reduce stiffness through gentle, repetitive motion.
- Build endurance without pounding on joints.
Helpful Tip: Start with short intervals and take standing breaks against the wall to keep your joints relaxed. Small, steady reps beat heroic efforts.
Gentle Range-of-Motion Movements
These are slow, supported movements that help keep joints mobile without forcing excessive range of motion. Your physical therapist may guide shoulder circles, hip swings, knee bends, or ankle mobility drills, depending on how your body feels that day.
Helpful Tip: Move to the point of an easy stretch, then come back. A rheumatoid arthritis-friendly motion should feel smooth. Remember, the goal is steady progress, not “pushing through.”
Leg Lifts with Water Support
Leg lifts in the pool can improve range of motion and strengthen hips and thighs while keeping impact low. You may use a wall, a noodle, or shallow water positioning to support good form.
Common options include:
- Side leg lifts for hip stability.
- Backward leg lifts for glutes.
- Controlled knee lifts to support walking mechanics.
Helpful Tip: Keep your trunk tall and move slowly so the work stays in your hips, not your lower back. If your back is doing the brunt of the work, it will file a complaint later.
Arm Resistance Sweeps
Upper-body weakness and changes in posture can creep in when pain limits activity. Water resistance allows for strengthening the shoulders, upper back, and arms without heavy equipment.
Your physical therapist may use:
- Horizontal sweeps across the body.
- Gentle push-pulls forward and back.
- Scapular, or shoulder blade, setting exercises for posture support.
Helpful Tip: Keep your shoulders down and breathe steadily. The neck has a way of volunteering for work that was not assigned.
Floating Core Exercises
Core work doesn’t have to mean floor exercises that irritate wrists, knees, or hips. In the pool, core training can feel more comfortable while still building trunk stability.
Your therapy might include:
- Supported marching.
- Gentle pelvic tilts.
- Balance holds with a flotation tool.
You may be surprised by how much your core has to work in the pool. The water helps hold you up, but it also adds a gentle wobble, keeping your stabilizing muscles switched on and doing the heavy lifting behind the scenes.
Benefits of Aquatic Therapy for People with Rheumatoid Arthritis
Clinical guidelines support low-impact exercise as part of comprehensive arthritis care, and many people find the pool is where that recommendation finally feels doable. When pain or fear has been holding them back, patients often report they can move more than expected in the water. Warm-water programs have also been linked to improvements in pain, function, and movement tolerance in patients with inflammatory arthritis.
With consistent guidance, benefits may include:
- Reduced joint swelling and stiffness.
- Improved functional mobility, including walking, transfers, and stairs.
- Better endurance with less fatigue.
- Increased confidence in moving with less pain.
- Support during flare-up recovery and return-to-exercise phases.
Those wins add up over time. Even small improvements, like standing longer to cook or walking more comfortably through a store, can make daily life easier.
Innovative Therapies for Complex Needs
Our specialized programs are designed to address unique health challenges.
How Physical Therapists Customize Aquatic Programs
When treating rheumatoid arthritis, your Ivy Rehab physical therapist understands that one patient’s “good day” can look completely different from another’s. That’s why expert guidance matters. They’ll build a plan that adjusts to your symptoms in real time, instead of asking you to follow a one-size-fits-all routine.
When administering water therapy for arthritis pain, guidance often includes:
- Adjusting intensity based on flare-ups and fatigue.
- Monitoring joint alignment and comfort throughout each movement.
- Modifying resistance by changing water depth, speed, or equipment.
- Integrating breathing, pacing, and relaxation strategies to reduce guarding.
A simple progression over time typically follows: mobility first, then strength, and finally function. When you’re ready, your therapist can help you transition from pool to land-based physical therapy.
Safety Tips for Patients Using Aquatic Therapy
Aquatic therapy is considered safe and effective, but rheumatoid arthritis responds best with smart pacing. Ultimately, you should leave feeling better than when you arrived.
Keep these precautions in mind, especially if you’re using hydrotherapy for arthritis pain during a sensitive period:
- Avoid high-intensity movements during flare-ups.
- Move slowly, focusing on comfort and control.
- Stay hydrated (yes, even in the pool).
- Keep exercises short if fatigue begins to set in.
- Use your physical therapist for guidance on proper form.
If you notice increased sharp pain or symptoms beyond normal post-exercise soreness, inform your physical therapist so they can make an immediate adjustment.
When Aquatic Therapy Is Especially Helpful for Rheumatoid Arthritis
Aquatic therapy is beneficial at various stages of care, but it’s particularly helpful when land-based movement becomes too challenging. It may be a strong option if you’re dealing with:
- Moderate to severe joint stiffness.
- Difficulty tolerating land-based PT or gym exercise.
- Fear of falling due to instability or weakness.
- Chronic swelling or reduced mobility that makes daily movement hard.
- A flare-up recovery period that calls for a gentle return-to-motion plan.
For some patients, the pool is the doorway back to more mobility. Once confidence returns, land-based work becomes more approachable.
Why Choose Ivy Rehab for Aquatic Therapy?
Aquatic therapy is most effective when used as part of a comprehensive plan rather than a one-time visit to the pool. You’ll work one-on-one with a certified physical therapist with advanced training in aquatic therapy techniques, so every session is guided and driven by your goals.
Depending on location and pool access, your plan may include:
- Warm-water exercises that use buoyancy to reduce joint pressure.
- Coaching for form and pacing, especially when fatigue is a factor.
- A clear progression from pool to land-based exercise as you build strength and confidence.
If symptoms flare up, we adjust. If you’re ready to explore aquatic therapy, find a location near you.
Your Next Chapter: A Stronger, Steadier You
Living with arthritis can make movement feel complicated. However, the right environment and guidance can make all the difference. Aquatic therapy for rheumatoid arthritis offers a low-impact way to reduce stiffness, build strength gently, and practice functional movement with more comfort and confidence.
If you’re looking for a safer return to exercise after flare-ups or simply need a way to move that doesn’t aggravate your joints, water therapy for arthritis pain may be what you’ve been looking for, and Ivy Rehab therapy can help guide you.
Ready to give your joints a break and your body a boost? Find a location near you.
References
- American College of Rheumatology. “Exercise and Arthritis.” Updated Aug. 2025. Accessed Dec. 26, 2025. https://rheumatology.org/exercise-and-arthritis
- England, Bryant R., et al. “2022 American College of Rheumatology Guideline for Exercise, Rehabilitation, Diet, and Additional Integrative Interventions for Rheumatoid Arthritis.” Arthritis Care & Research (Hoboken). Aug. 2023;75(8):1603-1615. doi:10.1002/acr.25117. https://pubmed.ncbi.nlm.nih.gov/37227116/
- Arthritis Foundation. “In the Swim: Aquatic Exercise for Arthritis.” Aug. 15, 2022. Accessed Dec. 26, 2025. https://www.arthritis.org/health-wellness/healthy-living/physical-activity/other-activities/water-exercise-benefits-for-arthritis